Even some 30 years ago, osteochondrosis was associated exclusively with elderly people, whose joints become inactive and hurt with every movement. However, times have changed. Today, more and more people are changing hard physical labor to sedentary work at the computer, less and less monitor the quality of nutrition, and more and more often face osteochondrosis of the cervical spine. It is not for nothing that osteochondrosis is called "the disease of the century", and almost every person who has reached the age of 25 encounters the symptoms of this disease.
This insidious disease, starting with unpleasant pain in the neck area, very quickly leads to serious consequences in the form of hearing and vision impairment, as well as memory impairment up to its complete loss. That is why every person should know the causes of osteochondrosis and consult a doctor in a timely manner in case of unpleasant symptoms of the disease. We will talk about them in this article.
Causes of cervical osteochondrosis
Paradoxically, all our problems with the cervical spine begin in early childhood, or rather in elementary school, where the child's posture deteriorates and scoliosis develops. It is at this moment that the system for supporting the head by the spine is disrupted, in particular, by its thinnest and most vulnerable part - the cervical. The second key factor in cervical osteochondrosis, which originates in early childhood, is insufficient physical fitness, in particular, the weakness of the spinal muscles and the so-called muscle corset designed to support the spine.
These are the two most important causes of the disease. All the rest are heavy burdens on the weakened spine, provoking the development of the disease in quite young and healthy people. First of all, these include a sedentary lifestyle and lack of physical activity, in particular, work, which is associated with a long stay in one position. This is most typical for drivers and office workers who sit at the computer in shift. All this is complemented by overweight, which seriously increases the load on the spine.
Other causes of cervical osteochondrosis are:
- past spinal injuries;
- metabolic disorders;
- hereditary predisposition;
- great physical activity;
- constant nervous tension and stress;
- anomalies of the cervical spine;
- bad habits (holding the telephone receiver with your ear and shoulder).
The development of osteochondrosis
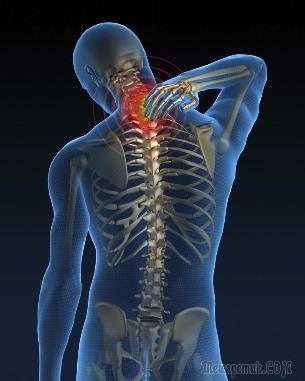
These unfavorable factors ultimately lead to an increase in the load on the cervical spine. When trying to compensate for the excessive load on the muscles of the neck, their spasm occurs, which leads to impaired blood circulation in this area and a decrease in metabolic processes. All this turns into the development of degenerative processes in the spine. First of all, the vertebrae begin to thin out and converge, squeezing their contents (annulus fibrosus) out of the spine. Such a protrusion in the language of doctors is called protrusion.
In the case of protrusion, the annulus fibrosus still retains its integrity, but the protrusion is already squeezing the blood vessels and nerves that run along the spinal column and feed the brain. Moreover, converging and deformed vertebrae begin to squeeze the roots of peripheral nerves, which leads to the development of the so-called "radicular syndrome", which manifests itself as severe pain in the back and neck. If you do not identify a problem (of which unpleasant symptoms will eloquently signal) and do not begin to treat osteochondrosis, the fibrous ring will rupture and a spinal hernia will appear. In this case, there will be serious problems with the nutrition of the brain.
Symptoms of cervical osteochondrosis
In its development, the disease goes through several stages, each of which has characteristic signs and symptoms. It should be noted here that osteochondrosis of the cervical spine differs from degenerative changes in other parts of the spine. The distances between the vertebrae are minimal here, and therefore even small degenerative changes cause unpleasant symptoms and lead to various complications.
1. Degree I osteochondrosis
This is the preclinical stage of the development of the disease, in which the patient experiences mild pain and discomfort during head turns, as well as tension and rapid fatigue in the neck and back during prolonged stay in one position (more often in a seated position). At this stage, osteochondrosis is perfectly treated by lifestyle changes, nutritional adjustments and regular exercise.
2. Degree II osteochondrosis
At this stage, instability appears between the vertebrae in the neck. A person in this case is faced with intense pain that radiates to the shoulder, neck or arm. During tilts or turns of the head, the pain increases significantly, since, due to a decrease in the distance between the vertebrae, nerve endings begin to be pinched. The patient begins to tire quickly, his performance decreases, distraction, forgetfulness appears, and he suffers from headaches.
3. Degree III osteochondrosis
With the onset of the third stage of the disease, pain in the back and neck becomes even stronger, the mobility of the neck is noticeably reduced, and when the neck turns, the crunch of the vertebrae can be heard. At night, the patient's fingers begin to go numb (primarily the little finger and ring finger), which is why the person wakes up several times a night. Throughout the day, such patients have an unpleasant heaviness in the hands. And even a short conversation on the phone, in which a person is forced to hold the mobile near the ear, turns into unpleasant tingling and numbness in the fingers. All this indicates an increase in protrusion, and possibly the appearance of a hernia in the cervical spine.
4. Degree IV osteochondrosis
At the last stage of the disease, the vertebral discs are destroyed, which cease to perform their functions and begin to be replaced by connective tissue. A patient in this condition may experience a violation of coordination of movement, noise and maddening pulsation in the ears appear, headaches intensify, visual acuity and hearing decrease. In some cases, numbness of the tongue may occur.
Here it should be said that due to the compression of blood vessels, blood flow to the brain is disrupted. Because of this, the patient develops neurotic disorders such as insomnia, nervousness, irritability and resentment, frequent mood swings and inability to concentrate. Periodically there may be outbursts of anger or fear, melancholy and depression attack.
In the later stages of osteochondrosis development, severe vascular spasms can lead to the appearance of "flies" before the eyes, a feeling of instability on a hard flat surface, severe dizziness, migraines, nausea, vomiting and frequent fainting.
Disease Diagnostics
To identify the cause of the pathology, the patient describes the unpleasant symptoms of his condition to the doctor. After listening to the patient, the specialist sends him to one of the following research methods.
1. Radiography. Currently, this diagnostic method is considered uninformative, especially in the last stages of the development of the disease.
2. Ultrasonic duplex scanning. This method is used in cases where a specialist assumes a violation of blood flow in the arteries that provide nutrition to the brain. The study shows the speed of blood flow and determines if there are obstacles in its path.
3. CT (computed tomography). This method is more informative in comparison with radiography, since it not only reveals the problem, but also allows you to determine the presence and size of hernias, albeit with difficulty.
4. MRI (magnetic resonance imaging). The most informative method for diagnosing osteochondrosis today, which allows you to see the bone structures, the presence of hernias and even the direction of their development.
Treatment of osteochondrosis
Let's say right away that in order to deal with such a serious problem as osteochondrosis of the cervical spine, you should contact a neurologist. True, if the clinic has a vertebrologist, it is better to contact him first.
Osteochondrosis can only be treated in a complex manner. The complex of methods used includes drug therapy, massage of the cervical-collar zone, exercise therapy, physiotherapy methods, as well as proper nutrition. Only a combination of all these methods will help to cope with the disease and normalize the patient's well-being.
Help for severe pain
In the case of severe pain, doctors recommend taking drugs such as Analgin, Baralgin or Tempalgin. When these drugs no longer provide relief, you can switch to non-steroidal anti-inflammatory drugs.
In a general sense, drug therapy includes the following means:
- NSAIDs (non-steroidal anti-inflammatory drugs). These remedies eliminate pain, relieve swelling and cope with inflammation of the nerve roots.
- Chondroprotectors. Such drugs perfectly restore damaged cartilage tissue.
- Vitamins of group B. They are necessary to improve metabolic processes in nerve tissues.
- Muscle relaxants. These drugs work to reduce muscle spasms.
- Preparations that improve the rheological properties of blood. Thanks to such means, the supply of oxygen and nutrients to the brain and nerve endings is improved.
It should be noted here that it is possible to achieve a tangible effect in the fight against osteochondrosis with the help of ointments and tablets only if treatment with drugs is combined with other methods of therapy. Otherwise, the drugs will only have a temporary effect.
Many specialists tend to treat osteochondrosis with injections in order to quickly act on the nerve endings and save the patient from possible side effects when taking pills. However, vitamins are best taken orally becausevitamins are well absorbed by the body with any method of intake, but injections with them can be painful.
Physiotherapy treatments
Treatment with drugs must be combined with physiotherapy methods. The most effective for this disease are:
- Electrophoresis (in combination with drugs). In this case, medicines penetrate to the damaged vertebrae under the influence of an electric current.
- Ultrasound. This method of exposure allows you to remove the inflammatory process, relieve pain and improve metabolic processes in tissues.
- Magnetotherapy. This type of physiotherapy relieves puffiness and pain.
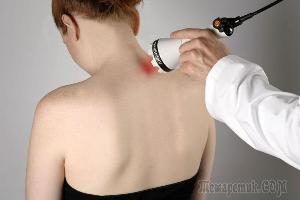
- Laser therapy. It is an excellent method of fighting inflammation and improves blood circulation.
Diet for osteochondrosis
The restoration of the affected vertebrae also includes a special diet that normalizes metabolic processes in the body, prevents salt deposition, nourishes and restores cartilage tissue, and also strengthens the ligaments between the vertebral discs.
To achieve this, first of all, the following should be excluded from the patient's diet:
- alcoholic beverages;
- fatty and fried foods;
- spicy and too salty foods;
- strong broths;
- weaknesses and baked goods;
- strong tea and coffee;
- pickles and marinades;
- canned products.
The diet of a patient with osteochondrosis should consist of the following foods:
- lean meat and fish;
- low-fat milk, cottage cheese and kefir;
- butter (small amount);
- whole grain cereals and soups;
- jellied meat, aspic from fish or meat;
- vegetables, fruits and berries;
- juices, fruit drinks, jelly and compotes.
When osteochondrosis is localized in the cervical spine, it is important to adhere to the drinking regime, drinking at least 1. 5 liters of water per day. If you are overweight, then you should think about how to get rid of those extra pounds, which put additional stress on the spine. It is advisable to switch to meals 5 times a day in small portions.
At the same time, as can be seen from the list of permitted foods, the basis of food should be low-fat vegetarian soups, boiled lean meat, fish, seafood, unsweetened vegetables and fruits.
A sample menu for the day will look like this:
- breakfast: cottage cheese, a couple of apples, tea without sugar;
- lunch: baked pear, some oatmeal cookies;
- lunch: vegetarian borscht, boiled chicken with vegetable salad;
- afternoon snack: dry biscuits and fruit juice;
- dinner: baked fish with vegetables and tea without sugar.
Exercise therapy for osteochondrosis
Physical education gives tremendous results in the treatment of osteochondrosis, although it is possible to do gymnastics for the cervical spine only during the recovery period. It is important here that in the process of massage or gymnastics the patient does not experience discomfort and pain.
Here are some of the most effective gymnastic exercises aimed at strengthening the cervical muscles and improving blood circulation in this area.
Exercise # 1
Lying on your stomach and resting your hands on the floor, slowly raise your head and torso so that your back remains straight. Hold this position for 1 minute, then return to the starting position. The element is repeated 2-3 times.
Exercise # 2
Lying on your stomach and stretching your arms along your body, slightly raise your head and start turning it first to the right, trying to touch the floor with your ear, and then to the left. Make 6 turns in each direction.
Exercise # 3
Sitting on the floor, while inhaling, bend forward, trying to reach your chest with your chin, and as you exhale, return to the starting position and tilt your head back. Repeat the element 10-15 times.
Exercise # 4
Place your palms on your forehead and try to press hard on your head. At the same time, while straining the muscles of your neck, resist your hands, preventing you from tilting your head. Hold the pressure for 20-30 seconds, then lower your arms and relax. Repeat the element 2-3 times, and then repeat the exercise in the opposite direction, bringing the clasped hands to the back of the head.
Exercise # 5
Start slowly rotating your head to the right and left, trying to look behind your back. Make 10 turns to each side.
















































